ABC Imagem Cardiovasc. 2026; 39(1): e20250030
Coexistence of Partial Anomalous Pulmonary Venous Connection and Coronary Artery Fistulas: A Rare Case Report
DOI: 10.36660/abcimg.20250030i
Abstract
Background
Dyspnoea is a common clinical symptom that frequently prompts hospital admission and is associated with significant morbidity. While it most often results from prevalent cardiopulmonary conditions, rare congenital cardiovascular anomalies can also manifest with dyspnoea. Partial Anomalous Pulmonary Venous Connection (PAPVC) and Coronary Artery Fistulas (CAFs) are uncommon congenital malformations of the cardiovascular system, and their simultaneous presence is exceedingly rare. Early recognition of such anomalies is critical to avoid progressive hemodynamic compromise and to guide appropriate management strategies.
Case Presentation
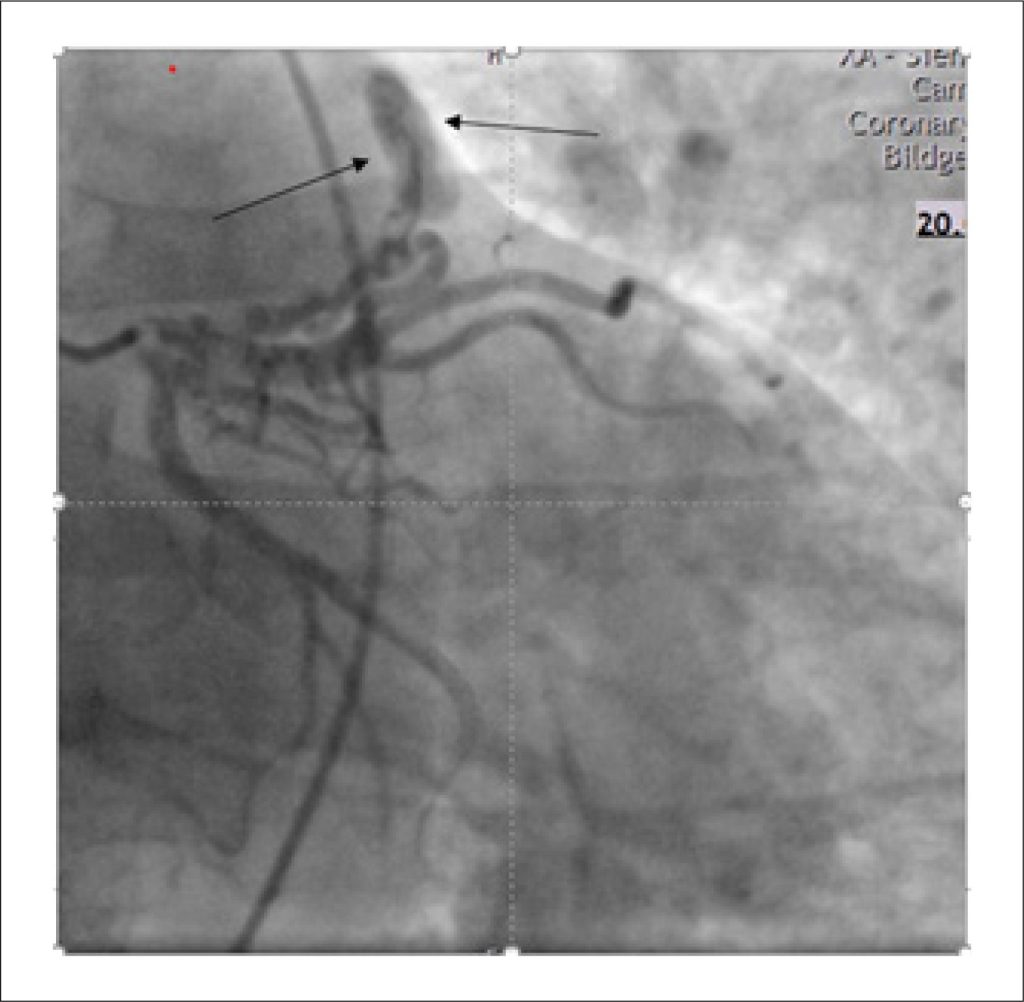
We present the case of a 55-year-old man who experienced an acute onset of dyspnoea lasting approximately two hours. Initial clinical assessment and routine investigations—including physical examination, echocardiography, electrocardiography, and right and left heart catheterization—raised suspicion of an underlying cardiac abnormality, prompting further evaluation. Subsequent cardiac Magnetic Resonance Imaging (MRI) and Multi-Detector Computed Tomography (MDCT) revealed the presence of a Partial Anomalous Pulmonary Venous Connection (PAPVC) accompanied by Coronary Artery Fistulas (CAFs). Given the non-complex characteristics of the shunt in this case, a shared decision was reached with the patient to proceed with conservative management.
Discussion
PAPVC and Coronary Artery Fistulas CAFs are rare entities that should be considered in the differential diagnosis. However, recommending their evaluation as initial diagnostic hypotheses may result in unnecessary investigations.
Keywords: Coronary vessels; Differential Diagnosis; Echocardiography
240