Arq Bras Cardiol: Imagem cardiovasc. 2023; 36(2): e20230019
Transient Perivascular Inflammation of the Carotid Artery (TIPIC): Vascular Ultrasonography Role
DOI: 10.36660/abcimg.20230019i
Case Report
Male patient, 53 years old, complaining of progressive unilateral neck pain, which appeared spontaneously, in association with edema, local redness, and great sensitivity to palpation. The patient’s past history included radiotherapy for about 5 years in the neck and face region, on the opposite side of the current complaint. The patient was a non-smoker and had no other significant risk factors for atherosclerotic disease. One year before the current clinical picture, the patient had undergone VUS of the carotid arteries, in a routine evaluation for follow-up after radiotherapy, the result was within normal limits.
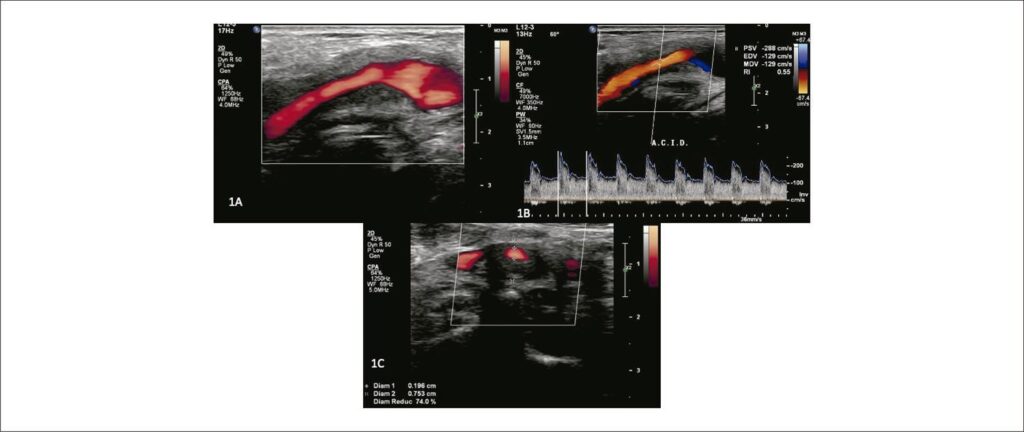
Given the clinical picture, a new VUS examination was requested, which included the standard protocol for evaluating the extracranial common, external, and internal carotid arteries (ACC, ICA and ACE). Special attention was given to extracarotid (perivascular) tissues due to the history of radiotherapy. The B-mode US showed extensive hypoechoic and homogeneous involvement of the tissues, including the arterial wall at the level of the carotid bifurcation, expanding to the proximal ICA (). The peak systolic velocity and end-diastolic velocity (PSV/EDV) were high: PSV/EDV = 288/129 cm/s (). Local stenosis measured in the transverse plane of the image was estimated at 74% (), consistent with the Doppler velocity data. The extent of the affected area was 5.57 mm compared to a lumen of 1.96 mm. Magnetic resonance imaging (MRI) and angioresonance (MRA) showed irregular thickening, with contrast enhancement, in the proximal ICA and bifurcation, corroborating the VUS findings ().
[…]
Keywords: arteritis; Carotid artery
399