Arq Bras Cardiol: Imagem cardiovasc. 2023; 36(2): e20230027
Pulmonary Congestion in Heart Failure With Reduced Ejection Fraction: Comparison Between Lung Ultrasound and Remote Dielectric Sensing
DOI: 10.36660/abcimg.20230027i
Abstract
Backgound
Outpatient assessment of pulmonary congestion in patients with heart failure with reduced ejection fraction (HFREF) can minimize hospitalizations due to decompensation and optimize the use of diuretics.
Objective
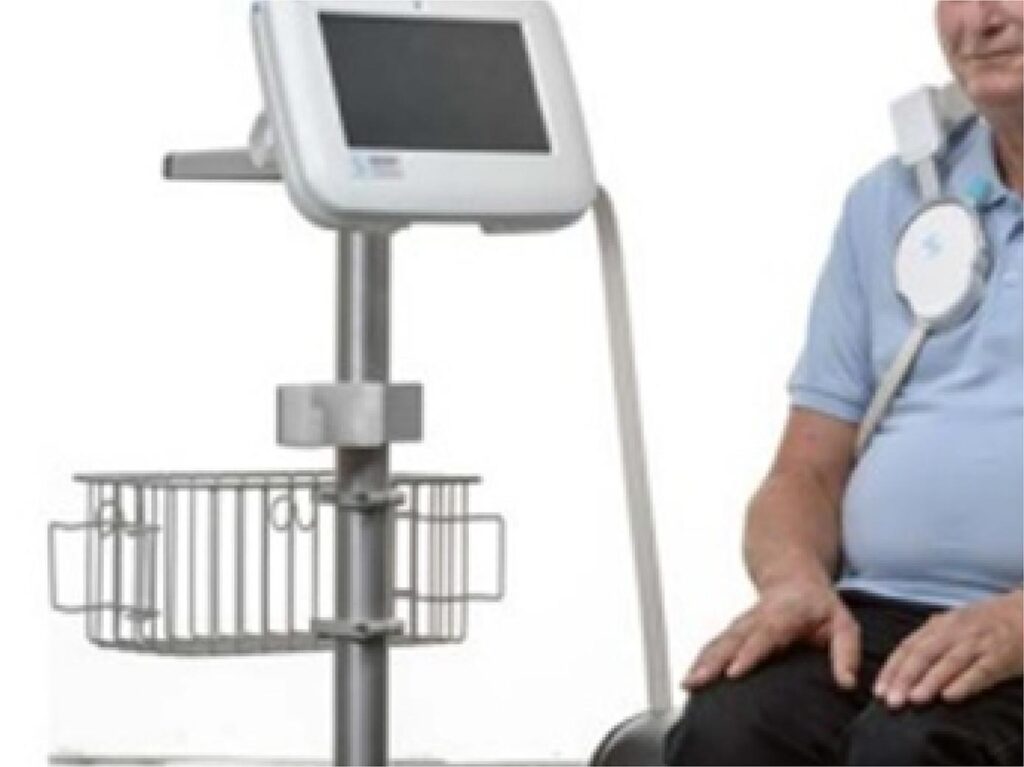
To compare the remote dielectric sensor (REDS), a validated device for detecting pulmonary extravascular fluid, with clinical parameters, transthoracic echocardiogram (TTE) and lung ultrasound (ULSP).
Methods
We included 38 patients from heart failure clinic (63±12 years; 21 men). All were submitted within 24 hours to clinical evaluation with description of paroxysmal nocturnal dyspnea, leg edema (LE), presence of dizziness; laboratory evaluation of NT-ProBNP; evaluation by REDS and TTE with analysis of parameters of systemic congestion by the inferior vena cava evaluation, function of the right ventricle and of pulmonary congestion, such as evaluation of filling pressures by average of E/e’ and indexed left atrial volume. The ULSP was performed using the 8 points anterior quadrants protocol, counting B lines in one respiratory cycle.
Results
22 patients had REDS ≥ 35% (indicative of pulmonary congestion) and 16 patients REDS<35%. Clinical and echocardiographic parameters were compared with REDS ≥ 35%. In the multivariate analysis, the variables body surface area, B lines and LE were associated with REDS ≥ 35%. NT-ProBNP was similar and elevated in both groups.
Conclusions
Outpatient monitoring of HFREF for volume control can be sensitized by the presence of B lines on the ULSP with good correlation to REDS ≥ 35%. NT pro BNP was not able to differentiate patients with congestion detected by REDS.
Keywords: Heart failure; Lung; Ultrasonography
1,319